Does Aetna Cover Outpatient Drug Rehab?
.jpg)
If you have Aetna and you are looking for IOP or PHP treatment in Virginia, the answer is yes — Aetna covers outpatient drug rehab. What varies is the cost-sharing structure, the prior authorization requirements, and which specific Aetna product you hold.
Here is the full picture — what Aetna covers, how authorization works, and how to confirm your benefits before starting treatment at Bold Recovery.
Does Federal Law Require Aetna to Cover Outpatient Rehab?
Yes. The Mental Health Parity and Addiction Equity Act (MHPAEA) requires Aetna — along with all major commercial insurers — to provide mental health and substance use disorder benefits that are no more restrictive than comparable medical or surgical benefits.
This means Aetna cannot apply lower visit caps, higher cost-sharing thresholds, or more burdensome prior authorization requirements to IOP or PHP than it does to equivalent medical services. Parity is a federal legal requirement, not a plan option.
What Does Aetna Cover for Outpatient Rehab?
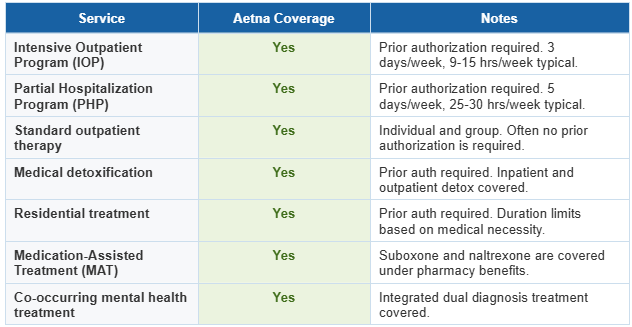
Aetna Commercial vs. Aetna Better Health of Virginia
Aetna operates two distinct insurance products in Virginia that affect your coverage differently:
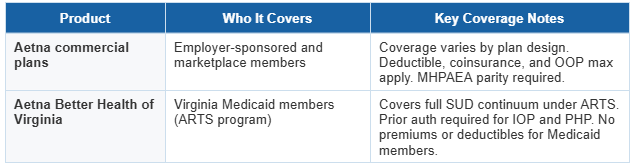
If you have Aetna through your employer or the marketplace, your cost-sharing structure applies. If you have Aetna Better Health through Virginia Medicaid, the ARTS benefit applies, which means comprehensive SUD coverage with no premium and typically no cost-sharing.
How Does Aetna Determine Medical Necessity for IOP?
Aetna uses clinical criteria — including Milliman Care Guidelines (MCG) and InterQual — to evaluate prior authorization requests for IOP and PHP. Medical necessity is established through a clinical assessment that documents:
- Substance use disorder diagnosis and severity level
- Prior treatment history and response
- Current level of functioning and daily impairment
- Safety and withdrawal risk
- Appropriate level of care recommendation from a licensed clinician
Bold Recovery's clinical team prepares this documentation as part of the standard intake and assessment process. Authorization submissions are handled on your behalf — you do not prepare paperwork.
What Affects Your Out-of-Pocket Cost With Aetna?
For commercial Aetna plans, your real cost depends on four variables:
- Whether you have met your annual deductible
- Your coinsurance rate after the deductible — typically 20% to 40% for in-network behavioral health
- Whether your provider is in-network with your specific Aetna plan
- Your plan's out-of-pocket maximum — which caps your total annual exposure
Bold Recovery confirms all four variables during the free benefits verification call — so you have exact numbers before treatment begins.
Take the First Step Today
If you’re ready to explore your options — or just want to ask questions — reach out today. We’ll guide you with clarity, compassion, and confidence.
.svg)
or message us directly through our website
You don’t have to figure this out alone. Let’s take the next step — together.
- Mental Health Parity and Addiction Equity Act (MHPAEA). (2008, as amended 2024). U.S. Department of Labor. Washington, D.C.
- Aetna Inc. (2024). Substance Use Disorder and Mental Health Coverage Summary — Commercial Plans. Hartford, CT.
- Virginia Department of Medical Assistance Services (DMAS). (2024). Aetna Better Health of Virginia — ARTS Program Coverage. Richmond, VA.
- American Society of Addiction Medicine (ASAM). (2023). The ASAM Criteria: Treatment Criteria for Addictive, Substance-Related, and Co-Occurring Conditions. 4th ed.
- SAMHSA. (2023). Coverage of Behavioral Health Services Under Commercial Insurance: A Guide for Consumers. Rockville, MD.
- Centers for Medicare and Medicaid Services (CMS). (2024). Mental Health Parity Implementation and Enforcement. Washington, D.C.
Frequently Asked Questions

Yes. Aetna covers both IOP and PHP in Virginia as medically necessary levels of care for substance use disorder. Prior authorization is required for both. Bold Recovery handles authorization on behalf of all clients. For Medicaid members, Aetna Better Health of Virginia covers the full SUD continuum under the ARTS program

Aetna commercial plans are employer-sponsored or marketplace plans with deductibles and coinsurance. Aetna Better Health of Virginia is the Medicaid managed care product that covers the full ARTS substance use disorder benefit with no premiums or deductibles for eligible members.

Aetna uses clinical criteria including Milliman Care Guidelines and InterQual to evaluate IOP and PHP authorization requests. Medical necessity is established through a clinical assessment documenting diagnosis, severity, prior treatment history, and level-of-care recommendation.







