Does Blue Cross Blue Shield Cover Rehab in Virginia?

If you have Blue Cross Blue Shield and you are looking for addiction treatment in Virginia, the direct answer is yes, BCBS covers rehab. The more important answer is: your specific coverage depends on your plan type, and verifying those details before you start is what turns coverage into treatment.
Here is what BCBS covers, how to understand your specific plan, and what Bold Recovery's admissions team does to make sure your benefits work for you.
Does Federal Law Require BCBS to Cover Rehab?
Yes. The Mental Health Parity and Addiction Equity Act (MHPAEA) — a federal law — requires insurance plans that cover mental health and substance use disorder services to provide those benefits at parity with medical and surgical coverage. BCBS plans sold or administered in Virginia must comply with MHPAEA.
This means BCBS cannot apply stricter limits — lower visit caps, higher copays, more restrictive prior authorization requirements — to addiction treatment than to comparable medical services.
What Does BCBS Cover for Addiction Treatment in Virginia?
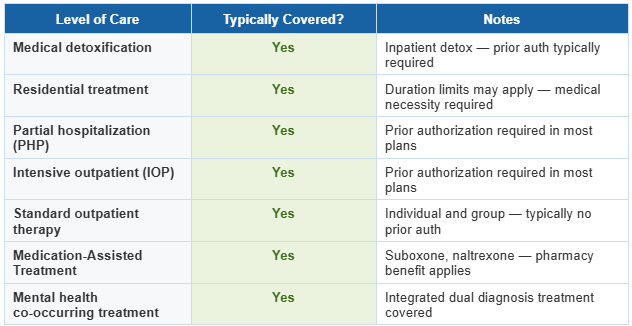
BCBS Plan Types in Virginia — What Affects Your Coverage
Not all BCBS plans are identical. Your specific out-of-pocket costs, prior authorization requirements, and network restrictions depend on your plan type:

Anthem Blue Cross Blue Shield in Virginia
In Virginia, Blue Cross Blue Shield plans are primarily administered through Anthem Blue Cross Blue Shield. Anthem is one of the largest insurers in Virginia and is in-network with Bold Recovery.
Key Anthem BCBS terms to know when verifying your rehab benefits:
- Deductible — the amount you pay out-of-pocket before insurance begins covering costs
- Out-of-pocket maximum — the cap on your total annual out-of-pocket spending
- Copay or coinsurance — your share of each covered service after the deductible
- In-network vs. out-of-network — whether your provider is contracted with your plan
- Prior authorization — the plan approval required before certain levels of care begin
These terms determine your real cost of treatment. Understanding them before you start prevents surprises.
How to Verify Your BCBS Rehab Coverage
The fastest and most accurate way to verify your BCBS coverage for addiction treatment in Virginia is to call Bold Recovery directly. Our admissions team will:
- Call your insurance plan on your behalf
- Verify which services are covered and at what cost-sharing level
- Confirm in-network status and prior authorization requirements
- Give you a clear out-of-pocket estimate before treatment begins
- Submit prior authorization on your behalf if treatment is recommended
You do not need to navigate insurance alone. That is part of what our admissions process does.
Take the First Step Today
If you’re ready to explore your options — or just want to ask questions — reach out today. We’ll guide you with clarity, compassion, and confidence.
.svg)
or message us directly through our website
You don’t have to figure this out alone. Let’s take the next step — together.
- Mental Health Parity and Addiction Equity Act (MHPAEA). (2008, as amended 2024). U.S. Department of Labor. Washington, D.C.
- Centers for Medicare and Medicaid Services (CMS). (2024). Mental Health Parity and Addiction Equity Act Compliance and Enforcement. Washington, D.C.
- American Society of Addiction Medicine (ASAM). (2023). The ASAM Criteria: Treatment Criteria for Addictive, Substance-Related, and Co-Occurring Conditions. 4th ed.
- Anthem Blue Cross Blue Shield of Virginia. (2024). Behavioral Health and Substance Use Disorder Benefits Summary. Richmond, VA.
- SAMHSA. (2023). Coverage of Behavioral Health Services: Fact Sheet for Consumers. Rockville, MD.
- U.S. Department of Labor. (2024). FAQs About the Mental Health Parity and Addiction Equity Act. Employee Benefits Security Administration.
Frequently Asked Questions

Yes. BCBS covers addiction treatment in Virginia including detox, residential treatment, PHP, IOP, outpatient therapy, and MAT. Federal law (MHPAEA) requires BCBS plans to cover mental health and substance use disorder services at parity with medical benefits. Specific coverage depends on your plan type.

Yes. Anthem Blue Cross Blue Shield — the primary BCBS affiliate in Virginia — covers both IOP and PHP as medically necessary levels of care. Prior authorization is required. Bold Recovery handles the authorization process for all clients

The fastest way is to call Bold Recovery directly. Our admissions team will contact your BCBS plan, verify your specific benefits and cost-sharing, confirm in-network status, and give you a clear out-of-pocket estimate before treatment begins — at no cost to you.

MHPAEA (Mental Health Parity and Addiction Equity Act) is a federal law that requires insurance plans to cover mental health and substance use disorder services at parity with medical and surgical benefits. This means BCBS cannot apply stricter limits to addiction treatment than to comparable medical services.
Related Blog Posts
.png)
How Long Does MAT Treatment Last?
Find out how long MAT treatment lasts in Virginia, what determines your duration, when tapering is appropriate, and how Bold Recovery structures your medication timeline.

Does Medicaid Cover Addiction Treatment in Virginia?
Find out exactly what addiction treatment Virginia Medicaid covers in 2026 — including detox, PHP, IOP, MAT, and residential — and how to verify your coverage at Bold Recovery.

PHP vs. Inpatient Rehab: What's the Difference?
Choosing the right level of care is one of the most important decisions in recovery. Two options come up often in that conversation — partial hospitalization programs (PHP) and inpatient rehab. They sound similar. They serve very different purposes.







