Does Medicaid Cover Addiction Treatment in Virginia?

For many people in Virginia, the assumption that they cannot afford addiction treatment is the only thing standing between them and getting help. That assumption is wrong — and it is Can youcosting people their recovery.
Virginia Medicaid covers a comprehensive range of addiction treatment services. The coverage is real, it is broad, and it is available to you right now.
The ARTS Program: Virginia's SUD Coverage Framework
Virginia's Medicaid addiction treatment coverage operates through the Addiction and Recovery Treatment Services (ARTS) program, which launched in 2017. ARTS was designed specifically to expand access to evidence-based substance use disorder treatment for Medicaid members across the state.
ARTS applies to all Virginia Medicaid managed care plans and covers the full continuum of addiction care — from detox through long-term outpatient support.
What Does Virginia Medicaid Cover?
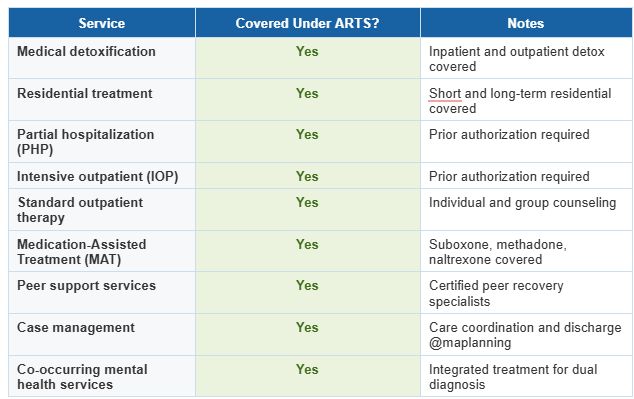
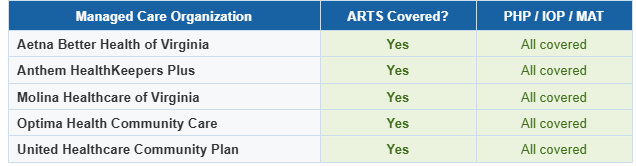
Which Virginia Medicaid Plans Cover Addiction Treatment?
All five Virginia Medicaid managed care organizations (MCOs) cover ARTS services. Your specific plan does not determine whether you are covered — it determines which providers are in-network and what the prior authorization process looks like.
How Does Prior Authorization Work?
Most levels of care above standard outpatient require prior authorization — a clinical review process where your Medicaid plan approves treatment before it begins. Prior authorization is not a barrier. It is an administrative step.
Bold Recovery's admissions team handles prior authorization on behalf of every client. You will not be asked to navigate insurance paperwork on your own. The process typically involves:
- A clinical assessment establishing medical necessity
- Submission of treatment request to your managed care plan
- Plan review and approval — typically within 1 to 3 business days for urgent cases
- Authorization confirmation before treatment begins
What If My Medicaid Coverage Is Denied?
Denial is not final. Virginia Medicaid members have the right to appeal coverage decisions — and most denials are resolved at the appeal stage when supported by proper clinical documentation.
Common reasons for denial include incomplete medical necessity documentation or a mismatch between the requested level of care and the initial assessment. Bold Recovery's clinical and admissions teams have direct experience resolving denials through the appeals process.
What About Medicare or Dual Eligibility?
If you have both Medicare and Medicaid — known as dual eligibility — your coverage is typically comprehensive. Medicare Part B covers outpatient behavioral health and MAT. Medicaid fills in cost-sharing gaps. Bold Recovery accepts both and handles coordination of benefits for dual-eligible clients.
Take the First Step Today
If you’re ready to explore your options — or just want to ask questions — reach out today. We’ll guide you with clarity, compassion, and confidence.
.svg)
or message us directly through our website
You don’t have to figure this out alone. Let’s take the next step — together.
- Virginia Department of Medical Assistance Services (DMAS). (2024). Addiction and Recovery Treatment Services (ARTS) Program Overview and Coverage Guidelines. Richmond, VA.
- SAMHSA. (2023). Behavioral Health Coverage in Medicaid. Substance Abuse and Mental Health Services Administration. Rockville, MD.
- Centers for Medicare and Medicaid Services (CMS). (2024). Medicaid Coverage of Substance Use Disorder Treatment. Washington, D.C.
- American Society of Addiction Medicine (ASAM). (2023). The ASAM Criteria: Treatment Criteria for Addictive, Substance-Related, and Co-Occurring Conditions. 4th ed.
- Virginia Medicaid. (2024). Managed Care Organization (MCO) Covered Services Comparison — ARTS Benefits. Richmond, VA.
- Mental Health Parity and Addiction Equity Act (MHPAEA). (2008, as amended 2024). Federal requirements for parity in mental health and substance use disorder benefits. U.S. Department of Labor.
Frequently Asked Questions

Yes. Virginia Medicaid covers addiction treatment through the ARTS program, including detox, residential treatment, PHP, IOP, standard outpatient, MAT (Suboxone, methadone, naltrexone), peer support, and case management. All five major Virginia Medicaid MCOs cover these services.

ARTS (Addiction and Recovery Treatment Services) is Virginia Medicaid's substance use disorder benefit program, launched in 2017. It provides comprehensive coverage for the full continuum of addiction treatment, from detox through long-term outpatient support, for all Medicaid members in Virginia.

Yes. Both IOP and PHP are covered under Virginia Medicaid's ARTS benefit across all five major managed care plans. Prior authorization is required, and Bold Recovery handles the authorization process on behalf of every client.

Denial is not final. Virginia Medicaid members have the right to appeal coverage decisions. Most denials are resolved at the appeal stage with proper clinical documentation. Bold Recovery's admissions team has direct experience navigating the appeals process.
Related Blog Posts
.png)
How Long Does MAT Treatment Last?
Find out how long MAT treatment lasts in Virginia, what determines your duration, when tapering is appropriate, and how Bold Recovery structures your medication timeline.


Can You Work While Attending an IOP Program?
Find out if you can work while in IOP in Virginia, how schedules are structured around employment, and what Bold Recovery's outpatient program looks like for working adults.







