What Is a Co-Occurring Disorder?

Addiction rarely arrives alone. Behind a substance use disorder — in a significant majority of people — there is at least one mental health condition operating simultaneously: depression, anxiety, PTSD, bipolar disorder, ADHD, or something else.
This is what clinicians call a co-occurring disorder. Understanding what it means, why it matters, and how it is treated is the difference between a treatment plan that addresses the full clinical picture and one that leaves half of it untouched.
The Plain-English Definition
A co-occurring disorder is the simultaneous presence of a substance use disorder (SUD) and at least one mental health condition. The terms dual diagnosis and comorbid disorder refer to the same clinical situation.
SAMHSA's 2022 National Survey on Drug Use and Health found that 21.5 million adults in the United States had both a substance use disorder and a mental health condition in the previous year. Among people actively seeking addiction treatment, more than 50% meet diagnostic criteria for at least one co-occurring mental health diagnosis.
This is not a rare complication of addiction. It is the statistical norm.
Why Do Mental Health Conditions and Addiction Co-Occur?
Three mechanisms drive the co-occurrence — and in most clinical presentations, all three are operating simultaneously:
1. Shared neurobiological vulnerability
Addiction and many mental health conditions share common neurobiological pathways — particularly dopamine, serotonin, and norepinephrine systems. A disruption in one system creates vulnerability in the other. Genetic factors that increase addiction risk also increase mental health risk.
2. Self-medication
Undiagnosed or undertreated mental health symptoms drive substance use. People use alcohol to manage anxiety, opioids to numb trauma responses, stimulants to compensate for ADHD-related dysregulation, and cannabis to reduce the hyperarousal of PTSD. The substances provide temporary relief while allowing the underlying condition to worsen.
3. Substance-induced psychiatric effects
Chronic substance use changes brain chemistry in ways that produce or worsen mental health symptoms. Alcohol depletes serotonin. Stimulants damage dopaminergic pathways. Opioid withdrawal activates anxiety and depressive symptoms. The psychiatric effects of substance use are real and clinically significant — distinct from the underlying condition, but often indistinguishable without clinical assessment.
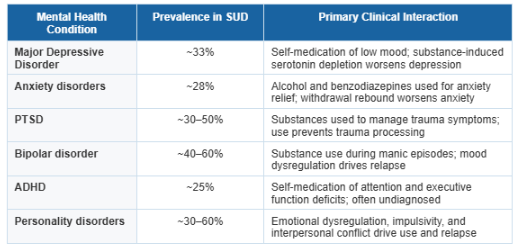
The Most Common Co-Occurring Disorders in Addiction Treatment
What Does Co-Occurring Disorder Treatment Look Like in Virginia?
Integrated co-occurring disorder treatment addresses both conditions simultaneously — within the same clinical program, by the same coordinated team. At Bold Recovery in Virginia, integrated treatment within IOP and PHP includes:
- Comprehensive psychiatric and addiction evaluation at intake — establishing the full diagnostic picture before treatment planning
- A unified treatment plan — specific clinical goals for both the SUD and the mental health condition
- Evidence-based therapy — CBT, DBT, trauma-focused therapy, or motivational interviewing depending on the clinical profile
- Psychiatric medication management — where co-occurring conditions require pharmacological support
- MAT integration — where opioid or alcohol use disorder co-occurs with the mental health condition
- Coordinated clinical team — psychiatrist and addiction clinician working from the same case formulation
Sequential treatment — addiction first, mental health second — is associated with significantly worse outcomes. The conditions maintain each other; treating them sequentially leaves each one without the intervention it needs at the critical moment.
Take the First Step Today
If you’re ready to explore your options — or just want to ask questions — reach out today. We’ll guide you with clarity, compassion, and confidence.
.svg)
or message us directly through our website
You don’t have to figure this out alone. Let’s take the next step — together.
- SAMHSA. (2023). Key Substance Use and Mental Health Indicators in the United States: Results from the 2022 NSDUH. HHS Pub. No. PEP23-07-01-006. Rockville, MD.
- Regier, D.A. et al. (1990). Comorbidity of mental disorders with alcohol and other drug abuse: Results from the Epidemiologic Catchment Area (ECA) Study. JAMA, 264(19), 2511-2518.
- American Society of Addiction Medicine (ASAM). (2023). The ASAM Criteria: Treatment Criteria for Addictive, Substance-Related, and Co-Occurring Conditions. 4th ed.
- National Institute on Drug Abuse (NIDA). (2024). Comorbidity: Substance Use Disorders and Other Mental Illnesses. Research Report. NIH.
- SAMHSA. (2020). Integrated Treatment for Co-Occurring Disorders Evidence-Based Practices (EBP) KIT. HHS Pub. No. SMA-08-4366. Rockville, MD.
- Drake, R.E. & Mueser, K.T. (2000). Psychosocial approaches to dual diagnosis. Schizophrenia Bulletin, 26(1), 105-118.
Frequently Asked Questions

A co-occurring disorder is the simultaneous presence of a substance use disorder and at least one mental health condition. Also called dual diagnosis or comorbid disorder, it affects more than 50% of people seeking addiction treatment. SAMHSA found 21.5 million US adults had both a SUD and mental health condition in 2022.

The most common co-occurring disorders in addiction treatment are major depressive disorder (33%), anxiety disorders (28%), PTSD (30-50%), bipolar disorder (40-60%), ADHD (25%), and personality disorders (30-60%).

Yes. Bold Recovery provides integrated co-occurring disorder treatment within IOP and PHP programs in Virginia. Every client receives a comprehensive psychiatric and addiction evaluation at intake. Both conditions are addressed simultaneously by a coordinated clinical team.

Yes. Federal mental health parity law (MHPAEA) requires insurance plans to cover mental health and substance use disorder treatment at parity with medical benefits. Virginia Medicaid and most commercial plans cover integrated co-occurring disorder treatment.
Related Blog Posts
.png)
How Long Does MAT Treatment Last?
Find out how long MAT treatment lasts in Virginia, what determines your duration, when tapering is appropriate, and how Bold Recovery structures your medication timeline.

Can You Treat Depression and Addiction at the Same Time?
Learn how Bold Recovery in Virginia treats depression and addiction simultaneously using integrated dual diagnosis programs — and why treating both at once produces better outcomes







